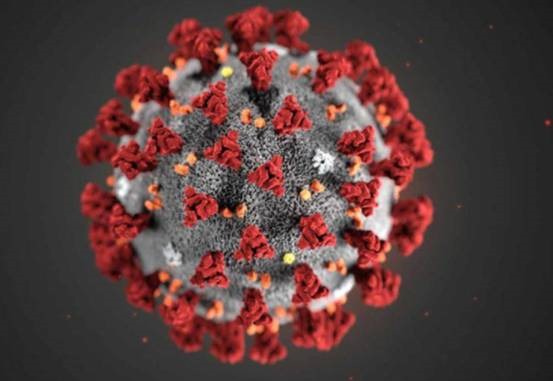
new strain of coronavirus pneumonia
AKA: Novel Coronavirus Pneumonia, Novel Coronavirus Pneumonia, NCP, Corona Virus Disease 2019, COVID-19, Novel Coronavirus Infections of Pneumonia
summarize
· Pneumonia due to novel coronavirus infection
· Fever, fatigue and dry cough at first, and gradually difficulty breathing
· Have the ability to transmit human to human and wear masks properly for added protection.
· Most have a good prognosis, but a few are critically ill and may even die.
Disease definition
Novel coronavirus pneumonia is an acute infectious pneumonia caused by a novel coronavirus not previously found in humans, the 2019 novel coronavirus, which was tentatively named “novel coronavirus pneumonia” by the National Health Commission on February 7, 2020. Corona Virus Disease 2019 (COVID-19) is the English name given by the World Health Organization (WHO) on February 11. The English name of “novel coronavirus pneumonia” is amended to “COVID-19”, which is consistent with the World Health Organization nomenclature, while the Chinese name remains unchanged.
On January 30, 2020, the WHO declared the novel coronavirus pneumonia outbreak a Public Health Emergency of International Concern (PHEIC).
The initial symptoms of the patients are mostly fever, fatigue and dry cough, and gradually severe manifestations such as dyspnea appear. The prognosis of most patients is good, and some severe cases may present with acute respiratory distress syndrome or septic shock, or even death. At present, effective antiviral drugs targeting pathogens are lacking, and isolation therapy and symptomatic support therapy are mainly used.
epidemiology
Based on current epidemiological investigations, the incubation period is 1-14 days, mostly 3-7 days. The incubation period is contagious and asymptomatic infected persons may also be the source of infection and the population is generally susceptible.
Transmission through respiratory droplets and close contact are the main routes of transmission. Since novel coronaviruses can be isolated in faeces and urine, attention should be paid to aerosol or contact transmission due to environmental contamination of faeces and urine. Aerosol transmission is possible through prolonged exposure to high aerosol concentrations in relatively closed environments. The risk of aerosol transmission may be present in confined, unventilated areas, and prevention and isolation treatments need to be strengthened.
· In December 2019, multiple cases of “unexplained pneumonia” were identified in Wuhan, Hubei Province, followed by patients with a history of exposure to seafood markets in South China or family gatherings.
· At 2100 hours on 7 January 2020, researchers detected a novel coronavirus in patient specimens.
· At 2400 hours on 10 January, nucleic acid testing for pathogens was completed.
· On 12 January, the World Health Organization (WHO) tentatively named the novel coronavirus responsible for the Wuhan pneumonia outbreak as 2019 novel coronavirus (2019-nCoV).
· On January 30, the WHO declared the novel coronavirus outbreak a public health emergency of international concern.
· On 7 February, the National Health and Wellness Commission decided to temporarily name “Novel Coronavirus Pneumonia”, or “NCP” for short. The English name is “Novel Coronavirus Pneumonia”, abbreviated as “NCP”.
· On February 11, WHO named the disease caused by the novel coronavirus Corona Virus Disease 2019, or COVID-19 for short.
Most frequently asked questions by patients.
What are the symptoms of a person infected with a novel coronavirus?
The severity of the symptoms of human infection with the novel coronavirus depends on the type of virus and the immune level of the human body, the common ones include fever, cough, shortness of breath or difficulty in breathing, more severe ones can lead to acute respiratory distress syndrome and septic shock, which can lead to death.
Can the new coronavirus be transmitted from person to person?
Yes, the novel coronavirus can be transmitted from person to person, and transmission usually occurs in homes, workplaces, crowded areas, or hospitals.
Is there a current vaccine for the novel coronavirus?
No. Emerging diseases may take longer to develop a vaccine for inoculation.
Is there a treatment for the novel coronavirus?
There is no specific treatment for diseases caused by novel coronavirus infections, and clinical treatment is based on symptomatic support therapy.
Are health care workers threatened by the new coronavirus?
Yes. Healthcare workers need to be in close contact with patients and are more susceptible to the threat of novel coronavirus infections. Therefore, the World Health Organization (WHO) recommends that health care workers strengthen their own infection prevention and control measures. Strict implementation of standard precautionary principles, personal protection, and hand hygiene will help prevent hospital-acquired infections to the greatest extent possible.
What can I do to protect myself?
As there is no effective treatment for this disease, prevention and isolation are the most effective ways to minimize contact with infected or potentially infected people. First of all, avoid going to crowded places and wear masks in public places. Next, pay attention to hand hygiene and dietary hygiene, wash hands frequently, drink plenty of fluids, avoid fatigue, ensure sleep, and keep more ventilation at home and in the workplace. If you have fever or cough, pay attention to cough etiquette, seek medical attention, and wear a mask on the way to the hospital.
cause of disease
· Novel coronavirus pneumonia is a new acute infectious disease.
· It is mainly caused by 2019 novel coronavirus (2019-nCoV) infection.
underlying cause
There are six coronaviruses that are known to infect humans, namely, HCoV-229E, HCoV-OC43, SARSr-CoV, HCoV-NL63, HCoV-HKU1, and MERSr-CoV.
The novel coronavirus (2019-nCov) belongs to the genus β and belongs to species 7, with genetic characteristics that are distinctly different from SARSr-CoV and MERSr-CoV.
causative factor
The elderly and those with underlying illnesses are sicker after infection.
symptom (of an illness)
According to the National Health Commission’s Diagnostic and Treatment Plan for Pneumonia in Novel Coronavirus Infection (Trial Seventh Edition), patients with heavy and critical types may have a moderately low fever or even no significant fever during the course of their illness. Patients of the light type only present with low fever and mild fatigue, and have no signs of pneumonia.
typical symptom
· Fever, fatigue and dry cough as the main manifestations.
· Few patients have symptoms such as nasal congestion, runny nose, sore throat and diarrhoea.
· In severe cases, dyspnea and/or hypoxemia most often develops one week after onset, and in severe cases rapidly progresses to acute respiratory distress syndrome, septic shock, uncorrectable metabolic acidosis and coagulopathy, and multiple organ failure.
seek medical treatment
This is an acute infection, often progressively worse in the first week, so seek immediate medical attention if.
· Recent onset of unexplained fever, fatigue, cough.
· A history of residence or travel in Wuhan within two weeks prior to the onset of the disease.
· History of close contact with diagnosed patients two weeks prior to onset of illness.
· Aggregate onset (2 or more people).
During the visit, the doctor may ask the following questions to take an initial history, and the patient may prepare appropriate answers in advance.
· When do you experience fever, cough, and other symptoms?
· Where did you go and who did you meet before the onset of the disease?
· Is there anyone around you with similar symptoms?
· Is there difficulty breathing?
· What are the underlying illnesses?
Diagnostic criteria
According to the Diagnostic and Treatment Protocol for Pneumonia with Novel Coronavirus Infection (Trial Version 7), issued by the National Health Commission of China.
suspected case
Combination of the following epidemiological history and clinical presentation: any one of the following epidemiological histories is present and any two of the clinical presentations are met. In the absence of a clear epidemiological history, 3 of the clinical manifestations are met.
epidemiological history
· A history of travel or residence in and around Wuhan, or other communities where cases have been reported, within 14 days prior to the onset of the disease.
· Had contact with a patient with fever or respiratory symptoms from the city of Wuhan and surrounding areas, or from a community where the case has been reported, in the 14 days prior to the onset of the disease.
· History of contact with a person infected with a novel coronavirus (nucleic acid test positive) within 14 days prior to onset of illness.
· Aggregate morbidity.
clinical manifestation
· Fever and/or respiratory symptoms.
· Have the above imaging features of pneumonia.
· Early in the course of the disease, the total number of white blood cells is normal or decreased, or the lymphocyte count is decreased.
Diagnosed cases
Suspected cases with evidence of one of the following etiologies.
· Real-time fluorescence RT-PCR for nucleic acid positive detection of novel coronavirus.
· Viral gene sequencing, highly homologous to known novel coronaviruses.
Clinical typing
light (machinery, aircraft etc)
Clinical symptoms were mild and there were no signs of pneumonia on imaging.
regular type
With fever and respiratory symptoms, pneumonia is visible on imaging.
heavy duty
An adult satisfies any of the following.
· Respiratory distress with a respiratory frequency of ≥ 30 breaths/min.
· (a) Resting means oxygen saturation ≤ 93%.
· Arterial partial pressure of oxygen (PaO₂)/oxygen uptake concentration (FiO₂) ≤ 300 mmHg (1 mmHg = 0.133 kPa), at high altitudes (over 1000 m above sea level) PaO2/FiO2 should be corrected according to the following formula: PaO2/FiO2 × [atmospheric pressure (mmHg)/760] .
In addition, those whose lung imaging shows significant lesion progression >50% within 24-48 hours are managed as heavy.
The child meets any of the following criteria.
· the presence of shortness of breath (<2 months of age, RR ≥ 60 beats/min; 2-12 months of age, RR ≥ 50 beats/min; 1-5 years of age, RR ≥ 40 beats/min; >5 years of age, RR ≥ 30 beats/min), except for the effects of fever and crying.
· (a) Oxygen saturation ≤92% at resting state.
· Assisted respiration (moaning, flaring of the nose, triple concave sign), cyanosis, intermittent apnea; lethargy, seizures.
· Refuses food or has difficulty feeding, with signs of dehydration.
critically ill
Any of the following.
· (a) Respiratory failure and the need for mechanical ventilation.
· (a) The occurrence of shock.
· Concomitant other organ failure requires ICU monitoring.
Clinical early warning indicators for severe and critical cases
Adult heavy and critical clinical warning indicators.
· Progressive decline in peripheral blood lymphocytes.
· Progressive increase in peripheral blood inflammatory factors such as IL-6, C-reactive protein.
· Progressive increase in lactic acid.
· Intrapulmonary lesions progress rapidly in a short period of time.
Heavy and critical childhood clinical early warning indicators.
· Increased respiratory rate.
· Poor mental reaction, lethargy.
· Progressive increase in lactic acid.
· Those whose imaging shows bilateral or multiple lung lobe infiltrates, pleural effusions, or rapid progression of the disease over a short period of time.
· Infants under 3 months of age or those with underlying diseases (congenital heart disease, bronchopulmonary dysplasia, respiratory malformations, abnormal hemoglobin, severe malnutrition, etc.), immunodeficiency or hypoplasia (chronic use of immunosuppressants).
Departments
Fever Clinic, Infection Unit, Intensive Care Unit.
Related checks
Doctor checkups
The main focus is on the lungs for the appropriate examination, listening for breath sounds, etc.
laboratory tests
· (a) Normal or decreased total peripheral white blood cell count and decreased lymphocyte count early in the course of the disease.
· Elevated liver enzymes, lactate dehydrogenase (LDH), myosin and creatine kinase in some patients.
· (a) Increased troponin is seen in some critically ill patients.
· Elevated C-reactive protein (CRP) and sedimentation rate and normal calcitonin levels in most patients.
· In severe cases, D-dimer elevation and progressive reduction of peripheral blood lymphocytes are present.
radiographic examination
In the early stage, there are multiple small patchy shadows and interstitial changes, which are obvious in the outer pulmonary band. In severe cases, there may be solid changes in the lung, and pleural effusion is rare.
Special inspections
Pathogen detection by collecting specimens of throat swabs, sputum or lower respiratory secretions for real-time fluorescence RT-PCR, which results in a positive nucleic acid test for the novel coronavirus. Or pathogen gene sequencing suggests a high degree of homology to the novel coronavirus. To improve the positive nucleic acid test rate, it is recommended that sputum be retained as much as possible, and lower respiratory secretions be collected from patients with tracheal intubation and sent for examination as soon as possible after specimen collection.
differential diagnosis
The doctor will conduct a detailed examination in several areas to determine.
· Light manifestations of novel coronavirus infection need to be distinguished from upper respiratory tract infections caused by other viruses.
· (a) Novel coronavirus pneumonia is primarily identified with other known viral pneumonia and mycoplasma pneumoniae infections, such as influenza virus, adenovirus and respiratory syncytial virus, especially in suspected cases, where possible, including rapid antigen testing and multiple PCR nucleic acid testing for common respiratory pathogens.
· It must also be distinguished from noninfectious diseases such as vasculitis, dermatomyositis, and organic pneumonia.
cure
Currently, there is a lack of effective antiviral drugs that target pathogens, and isolation and symptomatic support therapy are the mainstay of treatment.
According to the “Diagnostic and Treatment Plan for Pneumonia with Novel Coronavirus Infection (Trial Version 7)” issued by China’s National Health and Wellness Commission: for severe and critical cases, on the basis of symptomatic treatment, active prevention and treatment of complications, treatment of underlying diseases, prevention of secondary infections, and timely organ function support. Treatment is provided in the following ways.
· Respiratory support: includes oxygen therapy, high-flow nasal catheter oxygen therapy or noninvasive mechanical ventilation, invasive mechanical ventilation, and salvage therapy. Salvage therapy is for patients with severe ARDS and pulmonary resuscitation is recommended. With adequate human resources, prone ventilation should be performed for more than 12 hours per day. If prone ventilation is ineffective, extracorporeal membrane pulmonary oxygenation (ECMO) should be considered as soon as possible, if possible.
· Circulatory support: based on adequate fluid resuscitation, improve microcirculation, use vasoactive drugs, and perform hemodynamic monitoring if necessary. Perform noninvasive or invasive hemodynamic monitoring, and pay attention to fluid balance strategies to avoid over and underdose during resuscitation.
· Renal failure and renal replacement therapy: In addition to finding the cause of renal impairment, continuous renal replacement therapy (CRRT) may be an option for critically ill patients with renal failure.
· Plasma therapy for recovered persons: recommended for patients with rapidly progressing, heavy and critical disease. Dosage and dosage refer to the Clinical Treatment Plan for Recovered Plasma of New Coronary Pneumonia Patients (Trial First Edition).
· Blood purification therapy: blood purification system including plasma replacement, adsorption, perfusion, blood/plasma filtration, etc., can remove inflammatory factors, thus reducing the inflammatory response to the body’s damage, and can be used for the early and mid-stage treatment of cytokine storms in heavy and critically ill patients.
· Other therapeutic measures: intravenous gammaglobulin may be considered as appropriate in children with heavy or critical cases. Patients with heavy or critical forms of pregnancy should be actively terminated, with caesarean section being the first choice. Patients often suffer from anxiety and fear, so psychological guidance should be strengthened.
Acute phase treatment
Patients with hypoxia and respiratory distress should be given prompt oxygen therapy (e.g., nasal catheter oxygenation, mask oxygenation) and noninvasive or invasive ventilator support if necessary.
General treatment
· Rest in bed, strengthen supportive therapy, ensure sufficient heat; pay attention to water and electrolyte balance, maintain internal environmental stability; closely monitor vital signs and finger oxygen saturation.
· Monitor blood, urine, C-reactive protein (CRP), biochemical parameters (liver enzymes, cardiac enzymes, renal function, etc.), coagulation, perform arterial blood gas analysis if necessary, and review chest imaging according to the condition.
· According to changes in oxygen saturation, effective oxygen therapy measures are given in a timely manner, including nasal catheter, mask oxygen administration, trans-nasal high-flow oxygen therapy if necessary, and non-invasive or invasive mechanical ventilation.
· Treatment with hydrogen-oxygen mixed inhalation gas (H2/O2: 66.6%/33.3%) is available on a conditional basis.
medication
· Antiviral therapy: alpha-interferon nebulization, lopinavir/ritonavir, ribavirin, chloroquine phosphate, and abidrol may be tried, and ribavirin is recommended in combination with interferon or lopinavir/ritonavir. It is important to be aware of the adverse effects, contraindications, and interactions with other medications of the above drugs.
· None of the trial drugs were administered for more than 10 days. It is recommended to further evaluate the efficacy of the currently tested drugs in the clinical application. It is not recommended to use three or more antiviral drugs at the same time, and should be discontinued if intolerable side effects occur.
· Antimicrobial therapy: avoid blind or inappropriate use of antimicrobials, especially in combination with broad-spectrum antimicrobials.
· Other: Glucocorticosteroids are administered for a short period of time (3-5 days) as appropriate under the supervision of a physician, depending on the patient’s degree of dyspnea and the progression of chest imaging.
· The treatment of maternal patients should take into account the number of weeks of gestation, the choice of drugs with as little fetal impact as possible, and the question of whether to terminate the pregnancy before proceeding with treatment, and be informed.
TCM treatment
There is a lack of evidence-based medical evidence to support the treatment of this disease in Chinese medicine at the moment. According to the “Diagnostic and Treatment Plan for Pneumonia with Novel Coronavirus Infection (Trial 6th Edition)” issued by the National Health Commission, localities can refer to the recommended plan for the identification and treatment of pneumonia according to the illness, local climate characteristics and different physical conditions. It is recommended to go to a regular medical institution for treatment under the guidance of a physician.
prognosis
The prognosis of the majority of patients is good, and a few are in critical condition, according to the cases admitted so far. The elderly and those with chronic underlying diseases have a poor prognosis. The clinical course of maternal cases with novel coronavirus pneumonia is similar to that of patients of the same age. Childhood cases are relatively mild.
(fig.) repercussions
According to the 2019 Novel Coronavirus Pneumonia Respiratory Rehabilitation Guidance.
· Mild isolation and general discharge patients: most patients have mild or no persistent residual lung function impairment and are less likely to develop physical dysfunction.
· Patients with severe/critical discharge: may have generalized weakness and shortness of breath leading to limitation of physical function, with pulmonary function showing restrictive dyspnea, consistent with changes in pulmonary fibrosis on chest CT scan, this change may persist.
The sequelae of the novel coronavirus pneumonia described above require extensive case summaries and observations.
rehabilitative
Individuals with severe disease may have pulmonary fibrosis and recovery may take longer.
complications (medicine)
Patients with severe cases may have a combination of acute respiratory distress syndrome, septic shock, uncorrectable metabolic acidosis, and coagulopathy.
everyday life
There is a lack of effective treatment for novel coronavirus pneumonia. Daily life management focuses on prevention of infection and effective isolation of suspected and confirmed cases.
home care
Family clustering of novel coronavirus pneumonia occurs, and suspected symptoms are promptly referred to an infectious disease unit and require isolation in a hospital with effective isolation and protective conditions.
Daily life management
catering
· Not consuming wild animals (i.e., game), and fully cooked poultry, meat, and eggs.
· (a) Nutritional care, avoiding a varied diet and ensuring a variety of food, especially fresh vegetables and fruits.
· Adopt good eating habits, eat on time and in quantity, and avoid overeating.
sports
Exercise actively to control your weight. In addition, moderate exercise helps boost the immune system.
way of life
· Abstaining from smoking and limiting alcohol.
· (a) Getting enough sleep, resting and avoiding late nights.
· Focus on mental health and attention to relieving tension and reducing stress.
Daily condition monitoring
Pay attention to the monitoring of body temperature, if there are symptoms such as fever, fatigue, cough and other symptoms of prompt medical consultation. If you have a history of living or traveling in the epidemic source area (Wuhan City) within two weeks before the onset of the disease, have a history of contact with confirmed or suspected patients, or show signs of collective illness, you should consult a doctor promptly and take the initiative to isolate them. The following precautions should be taken after discharge from the hospital according to the “Novel Coronavirus Pneumonia Treatment Plan (Trial 6th Edition)”.
· The designated hospitals should make good contact with the primary medical institutions in the patients’ places of residence, share medical records, and push the information of discharged patients to the neighborhood committees and primary medical and health institutions in the patients’ districts or places of residence in a timely manner.
· After the patient is discharged from the hospital, due to low immune function during the recovery period, there is a risk of infection with other pathogens, it is recommended to continue self-health monitoring for 14 days, wear a mask, live in a well-ventilated single room with conditions, reduce close contact with family members, share meals, good hand hygiene, and avoid going outside.
· It is recommended to follow up and follow up in the hospital in the 2nd and 4th week after discharge.
Special considerations
· The incubation period is 1-14 days, most often 3-7 days. The incubation period is contagious, and asymptomatic infected persons may also be a source of infection. Active isolation is required if there is a history of confirmed or suspected patient exposure, even if there is no fever or other symptoms at the moment.
· De-isolation requires a return to normal temperature for more than 3 days, significant improvement in respiratory symptoms, and 2 consecutive (at least 1 day apart) negative pathogen tests.
guard against
In the event of an epidemic outbreak of an infectious disease, the measures taken include those targeting the pathogen, the susceptible population, the route of transmission and the source of the disease.
There is no effective vaccine for novel coronavirus pneumonia at this time, and personal protection is the most practical approach, including staying away from crowded places, washing hands frequently, drinking plenty of fluids, and taking rest.
Specific means of prevention are as follows.
· Minimize going outside, avoid crowded places, and avoid close contact with anyone who has cold or flu-like symptoms.
· (b) Wearing a medical surgical mask or N95 mask when travelling to public places, for medical treatment and on public transport.
· Do not touch, buy or eat wildlife (i.e., game) and avoid unprotected contact with wildlife and poultry livestock.
· Hand hygiene, frequent hand washing, using hand sanitizer or soap, running water, or using alcohol-based hand sanitizers.
· Do not cover your hands when sneezing or coughing, but cover your mouth and nose with your elbow or a tissue.
· (b) Keeping the home and workplace clean, with frequent opening of windows and increased ventilation.
· (a) Drinking more water, resting more, avoiding overnight stays and moderate exercise to improve individual immunity; paying attention to nutrition and reasonable diet, with meat, poultry and eggs being adequately cooked for consumption.
· Prepare common supplies, such as a thermometer, disposable masks, and household disinfection supplies.
reference material
[1]WHO:https://www.who.int/internal-publications-detail/clinical-management-of-severe-acute-respiratory-infection-when-novel-coronavirus-(ncov)-infection-is-suspected.
[2] Pneumonia treatment protocol for novel coronavirus infection (pilot version 8)
[3] Bureau of Disease Prevention and Control, National Health Commission, Chinese Center for Disease Control and Prevention. Guidelines for public protection against pneumonia associated with novel coronavirus infection [M]. People’s Health Publishing House, Beijing, 2020:26.
[4] Chinese Society of Rehabilitation Medicine: 2019 Novel Coronavirus Pneumonia Respiratory Rehabilitation Guideline (First Edition)